About sepsis
Sepsis – a medical emergency
Sepsis is a life-threatening condition that occurs when the body’s response to an infection results in damage to its own tissues and organs. It can progress rapidly and lead to organ failure, septic shock and even death if not treated promptly. Sepsis can affect anyone, regardless of age or pre-existing conditions, and always begins with an infection.
Sepsis can be difficult to recognize in its early stages. However, rapid identification and immediate medical intervention are crucial to improving outcomes and saving lives.
On this page you will find concise and understandable information about sepsis – its causes, symptoms, treatment options and long-term consequences. Our aim is to raise awareness of this life-threatening disease and provide a better understanding of its impact.

Signs and symptoms
The early signs of sepsis can be subtle and are often mistaken for other illnesses such as colds or flu, which can lead to delays in diagnosis and treatment. As sepsis progresses, it can lead to septic shock, which is characterized by a sharp drop in blood pressure and insufficient blood flow to vital organs. This can lead to severe organ damage and ultimately to death.
Signs of sepsis in adults
Sepsis is often not manifested by a single symptom, but by a combination of various changes. If you feel unusually unwell, look out for the following signs:
- Fever or chills
- Confusion or disorientation
- Rapid and/or heavy breathing, shortness of breath
- Rapid pulse / palpitations
- Cold extremities, cool skin
- Muscle pain or an extreme feeling of illness
- Pale, clammy or marbled skin
- Reduced urine output
Signs of sepsis in children and infants
Sepsis can worsen very quickly, especially in young children and infants. Early symptoms in children can vary widely, making early recognition difficult. These early signs may include fever, lethargy, irritability, rapid or difficult breathing, decreased urine output, poor feeding and vomiting. Because these signs can easily be confused with other common childhood illnesses, it is important that caregivers and healthcare providers recognize the early warning signs of sepsis and act accordingly.
See a doctor immediately if you or your child has an infection and any of these symptoms, especially if you are worried or if your child does not get better after being seen by a doctor or nurse:
- abnormal behavior, unusual drowsiness, sluggishness, change in character
- Irritability and unusual crying, convulsions or seizures
- Rapid or labored breathing
- Fast or weak pulse
- Pale, blotchy or marbled skin
- Cold extremities, cool skin
- Reduced urine output or significantly less wet diapers for several hours
- Repeated vomiting or diarrhea over 24 hours
- Refusal to drink (if under 6 months old)
What is sepsis?
Sepsis explained in 3 minutes:
English
You are currently seeing a placeholder. To access the actual content, click on the button below. Please note that data will be passed on to third-party providers.
More information
You are currently seeing a placeholder. To access the actual content, click on the button below. Please note that data will be passed on to third-party providers.
More informationCauses
Sepsis can be caused by various types of infections, including bacterial, viral, fungal and parasitic infections. The vast majority of infections that lead to sepsis are acquired outside of medical facilities. The most common sources of infection include the lungs, e.g. pneumonia, the urinary tract, the abdomen and the skin, as well as infections caused by injuries or surgical wounds.
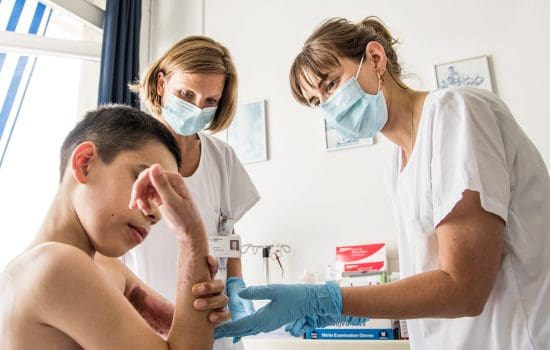
Risk factors
Sepsis can affect anyone, but certain groups are particularly at risk, including newborns, infants, the elderly and people with weakened immune systems. People with chronic conditions such as diabetes, cancer and kidney or liver disease are also at increased risk, as are people who have suffered severe burns or physical injuries. Sepsis survivors also have an increased risk of contracting sepsis again.
Persons at risk include
- Older adults (65 years and older)
- Infants and toddlers
- People with a weakened immune system, e.g. people undergoing chemotherapy or living with diseases such as HIV/AIDS or autoimmune diseases)
- Patients with chronic diseases such as diabetes, kidney disease or heart failure
- Hospitalized persons, especially those after major surgery, catheters or mechanical ventilators
- People with serious injuries, burns, trauma or open wounds
Prevention
The basis of sepsis prevention is to prevent infections from occurring in the first place. This includes regular hand washing, vaccinations according to the vaccination schedule, the correct intake of prescribed antibiotics or other anti-infectives, careful control of chronic illnesses such as lung or liver disease and diabetes, and careful wound care.
Responsible use of antibiotics
The responsible use of antibiotics is crucial in the fight against sepsis. Excessive and inappropriate use of antibiotics in healthcare and agriculture has contributed to the increase in antibiotic-resistant bacteria. To prevent this, it is important to use antibiotics only when absolutely necessary, keep the duration of treatment as short as possible and avoid unnecessary prescriptions. By using antibiotics prudently, we can maintain their effectiveness and reduce the risk of resistant infections that can lead to sepsis.
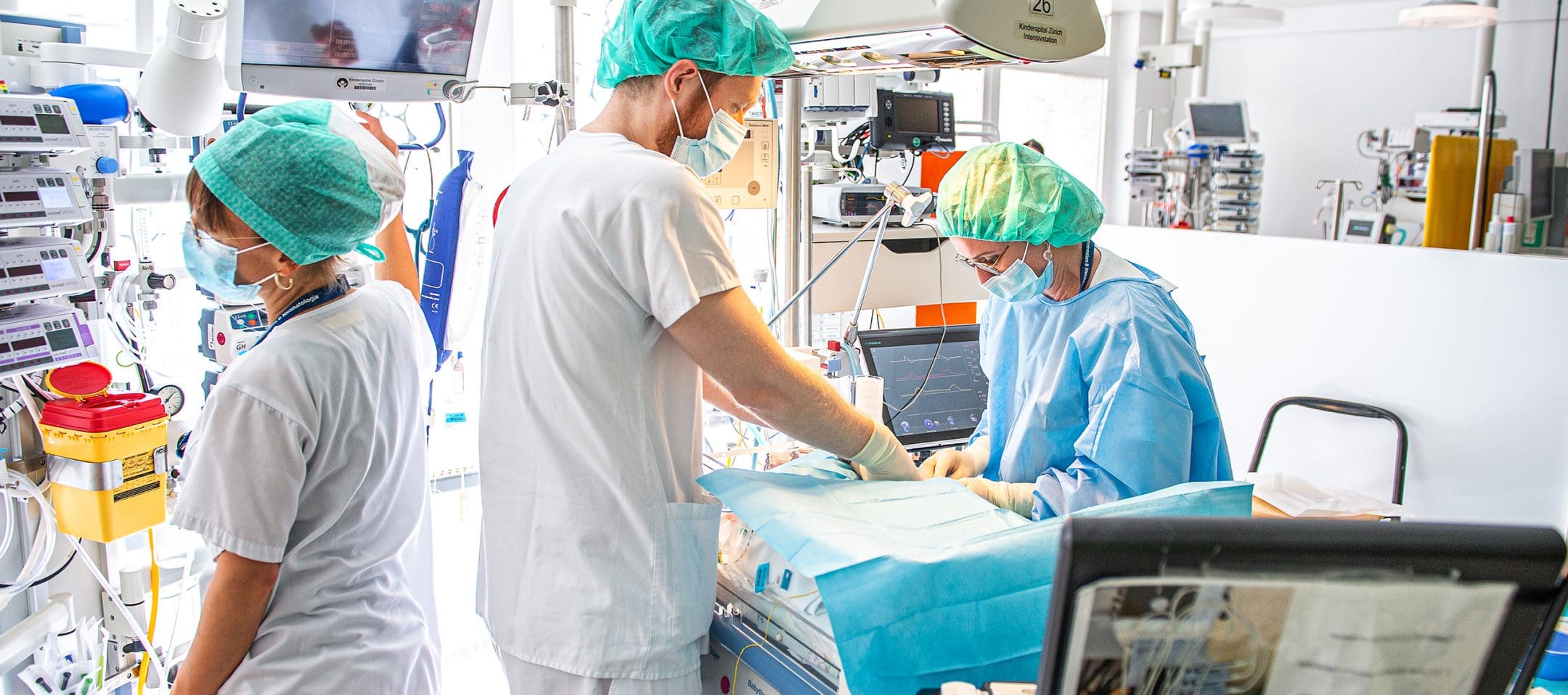
Treatment
Sepsis is a medical emergency that requires immediate attention and should be treated in hospital. Early detection and treatment significantly improves the chances of survival and reduces the risk of long-term complications.
Healthcare systems are encouraged to implement standardized protocols for sepsis treatment to improve patient outcomes. Monitoring and adjusting treatment based on the patient’s response is essential to address the dynamic and rapidly evolving nature of sepsis.
The most important elements of sepsis treatment include
- Antibiotics: Broad-spectrum antibiotics and, depending on the suspected diagnosis, other antimicrobial therapies are usually administered as soon as possible to combat the infection, often before laboratory results are available. These can be adjusted as the disease progresses, depending on the pathogen and clinical response.
- Fluid (infusion): Intravenous (IV) fluids are administered to maintain blood pressure and ensure adequate blood flow to vital organs.
- Vasopressors: If fluid alone is not enough to stabilize blood pressure, drugs known as vasopressors can be used to constrict the blood vessels and improve blood flow.
- Oxygen therapy: If breathing is impaired, additional oxygen or mechanical ventilation may be required.
- Surgical intervention: In some cases, surgical intervention may be necessary to eliminate the source of infection, e.g. by draining an abscess or removing infected tissue.
- Support for vital organs: This may include blood washing for kidney failure or medication to support heart function or other affected organs.
International treatment guidelines of the Surviving Sepsis Campaign:
Recovery and aftercare
For those who survive sepsis, the journey often does not end when they are discharged from hospital. Up to 50 percent of sepsis survivors suffer from long-term, sometimes lifelong health consequences. These include chronic pain, exhaustion, organ dysfunction and post-traumatic stress disorder (PTSD).

